Lupus pernio الذئبة التثليجية
HTML clipboard
INSTRUCTION
Look at this patient's face.
SALIENT FEATURES
History
-
Shortness of breath, cough, chest discomfort.
-
Fatigue, weight loss, malaise, anorexia .
Examination
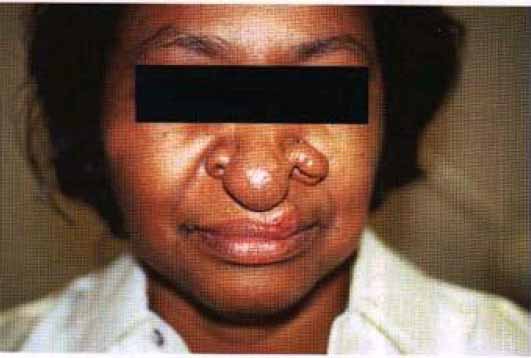
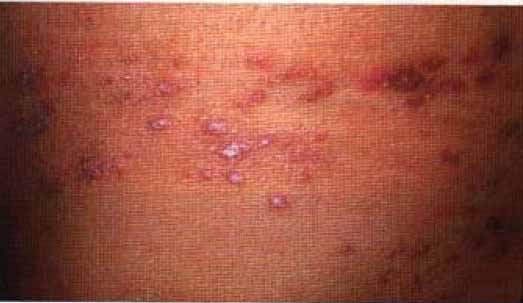
Reddish blue or violaceous plaques on the nose, cheeks, ears and fingers ,with telangiectasia over and around the plaques.
Proceed as follows:
Tell the examiner that you would like to do radiography for hilar adenopathy.
DIAGNOSIS
This patient has violaceous plaques on his face (lesion) due to sarcoidosis (aetiology) which are cosmetically disfiguring (functional status). (James DG & Jones Williams W1984 Sarcoidosis and other Graulomatous Disorders. Philadelphia: WB Saunders.)
ADVANCED-LEVEL QUESTIONS
What is the differential diagnosis of such a lesion?
-
Rhinophyma.
-
Lupus vulgans.
-
Leprosy.
What are the cutaneous manifestations of sarcoid ?
-
Erythema nodosum .
-
Micropapular sarcoid.
-
Scar infiltration.
-
Sarcoid plaques of limbs, shoulders, buttocks and thighs.
How may sarcoid present ?
-
Acute sarcoidosis usually presents in the third decade, characterized by erythema nodosum, parotid enlargement and hilar lymphadenopathy.
-
Chronic sarcoidosis usually presents in the fifth decade with an insidious onset characterized by fatigue, dyspnoea, arthralgia and lupus pernio. Bone cysts are another feature.
How would you investigate such a patient ?
-
FBC and ESR (leukopenia, eosinophilia and raised ESR).
-
CXR. There are three stages of sarcoidosis depending on the radiographic findings:
Stage I, bilateral hilar adenopathy alone;
Stage II, both hilar adenopathy and lung parenchymal involvement;
Stage III, parenchymal involvement alone.
-
Slit-lamp examination of the eyes.
-
Kviem's test (the antigen is cultured in human spleen and thus, increasingly, it is recommended that this test should not be performed because of the risk of trans-mitting viral infections).
-
Mantoux test (skin anergy is present in 70%).
-
Semm angiotensin-converting enzyme levels (raised in 40-80% with active disease, although this finding is neither sensitive nor specific enough to have diagnostic significance).
-
Lung function tests (usually restrictive changes with decreased lung volume sand diffusing capacity; occasionally airflow obstruction).
-
Serum calcium levels ( hypercalcaemia in 10% of patients).
-
Gallium-67 scan.
Bronchoalveolar lavage (usually characterized by an increase in lymphocytes and a high CD4:CD8 ratio).
Histological confirmation: transbronchial lung biopsy; biopsy of lymph node, skin ,liver, gums and minor salivary glands (presence of non-caseating granulomas with typical manifestations is generally required for diagnosis of sarcoidosis: fibrotic response develops over time).
What is the prognosis and treatment of sarcoidosis ?
-
Acute sarcoidosis usually regresses spontaneously within 2 years and does not recur; it may not require treatment.
-
Chronic sarcoidosis may require systemic cortiocosteroids in order to prevent serious disability and even death from respiratory failure.
What is the treatment of cutaneous sarcoid ?
Monthly intralesional triamcinolone injections, topical and systemic steroids .hydroxychloroquine, allopurinol, thalidomide, and tranilast (N Engl d Med 1997:336:1224-34).
What are the specific indications for systemic steroids in sarcoidosis?
-
Progressive deterioration in lung function, particularly transfer factor and vital capacity. Serial evaluation should be performed every 2 months initially, gradually increasing the intervals between follow-up to about 4-5 months; patients should be followed for at least 2 years after steroids are stopped.
-
CNS involvement.
-
Hypercalcaemia.
-
Severe ocular disease.
-
Hepatitis.
-
Cutaneous lesions.
-
Constitutional symptoms.
-
Symptomatic pulmonary lesions .
What are the ocular manifestations of sarcoidosis ?
-
Anterior uveitis, seen in about 5% of all cases:
- Acute.
-Chronic
- mutton fat keratic precipitates, iris nodules.
-
Retinal vasculitis, neo-vascularization (Bt J Ophthalmol 1981; 65: 348-58).
-
Vitreous opacities.
-
Choroidal granulomata.
-
Optic nerve granuloma.
What is Lofgren's syndrome ?
Erythema nodosum, hilar adenopathy and poly-arthralgias in a patient with sarcoidosis.
What is the source of the raised angiotensin-converting enzyme level in sarcoidosis ?
It is derived from the cell membranes of epithelioid cells in the sarcoid granuloma and its synthesis is controlled by epithelioid cells.
What is Blau's syndrome ?
It is a multi-system granulomatous disorder of the skin, eyes and joints that resembles childhood sarcoidosis. It was described by Edward Blau, a Wisconsin paediatrician (Lancet 1999; 354: 1035).
Is there any relationship between viral infections and sarcoid ?
Variant human herpes virus-8 DNA sequences have been found in sarcoid tissue. Also,16s ribosomal RNA genes of mycobacteria are more frequently found in sarcoid tissuebut this does not indicate infection by a particular mycobacteria species (Lancet 1997;350: 655-61).M.A. Kviem (b. 1892), a Norwegian pathologist.C.RM. Boeck (1845-1917), Professor of Medicine and dermatologist in Oslo, Norway,first described the disease as 'multiple benign sarcoid'.S. Lofgren, a Swedish physician.D. Geraint James, contemporary Professor of Medicine, Royal Free Hospital, London;his chief interest is sarcoidosis. His wife, Dame Sheila Sherlock, is a renownedhepatologist.C. Mantoux (1877-1947), a French physician from Cannes, who showed that hisintradermal test was more sensitive than the older Pirquet subcutaneous tests usingtuberculin.James DG & Jones Williams W (1984) Sarcoidosis and other Granulomatous DkorcharqPhiladelphia: WB Saunders.
