Xanthelasma اللويحة الصفراء
HTML clipboard
INSTRUCTION
Examine this patient's eyes.
SALIENT FEATURES
History
-
Jaundice, generalized pigmentation, itching (primary biliary cirrhosis).
-
Family history of hyperlipidaemia.· History of diabetes, hypertension.
-
Symptoms of hypothyroidism .
-
History of oral contraceptives.
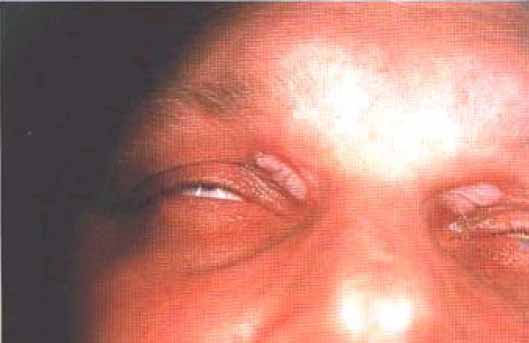
Examination
Xanthelasmata (fiat yellow nodules or plaques) seen on eyelids and around both eyes,particularly on the inner canthus .
Proceed as follows:
-
Look for the following signs:
- Corneal arcus.
- Jaundice, generalized pigmentation, scratch marks (primary biliary cirrhosis).
- Tendon xanthomata.
- Palmar xanthomata.
-
Tell the examiner that you would like to check the following:
- Urine sugar.
- Blood pressure.
-Pulse and ankle jerks (hypothyroidism).
Remember. Blood lipids can often be normal.
DIAGNOSIS
This patient has xanthelasmata on the eyelids (lesions) and I would like to test serumlipids to exclude an underlying lipid disorder (aetiology).
ADVANCED-LEVEL QUESTIONS
In which conditions are xanthelasmata seen?
Those in which there is an increase in serum cholesterol:
-
Type IIb hyperlipidaemia - increased cholesterol and triglycerides.
-
Type IIa hyperlipidaemia - increased cholesterol only.
-
Type Ili hyperlipidaemia - equal increase in cholesterol and triglycerides.
Mention a few secondary causes of hyperlipidaemia
.Diabetes mellitus, hypothyroidism, nephrotic syndrome, cholestatic jaundice, excessalcohol intake, oral contraceptives.
How would you manage a patient with hyperlipidaemia ?
-
Lifestyle advice.
-
Dietary modification (usually adequate for those whose cholesterol level is in therange 6.5-8 mmol/l).
-
Avoidance of alcohol, smoking, oestrogens and thiazides.
-
Exercise.
-
Control of hypertension and diabetes.
-
Lipid-lowering drugs.
Mention a few lipid-lowering drugs.
-
Ion exchange resin: colestyramine.
-
Fibrates:bezafibrate, gemfibrozil.
-
Sitostanol-ester margarine (a plant sterol that reduces serum cholesterolconcentration by inhibiting cholesterol absorption).
-
Hydroxymethylglutaryl (HMG) coenzyme A (CoA) reductase inhibitors:simvastatin, pravastatin, lovastatin. These drugs block the endogenous synthesis ofcholesterol and reduce levels of low-density lipoprotein cholesterol.
-
Nicotinic acid derivatives: nicotinic acid, probucol.
Are HMG CeA reductase inhibitors useful in patients with hypercholesterolaemia and coronary heart disease?
Yes, the Scandinavian SimvastatinSurvival Study (the 4S trial) demonstrated a survival benefit from lowering cholesterolwith simvastatin in patients with coronary disease (Lancet 1994; 344: 1383-9).
In theLIPID study (Long-Term Intervention with Pravastatin in Ischemic Heart Disease), amajor secondary prevention trial, pravastatin administered to 9000 patients withunstable angina or acute myocardialinfarction slgmncanUy reduced total mortality by 23%, coronary heart disease mortalityby 24%, the need for coronary revascularization, the number of admissions to hospitals(Lancet 2000; 355: 1871-5) and the risk of stroke by 20% (N Engl J Med 2000; 343:317-26). The Lescol in Severe Atherosclerosis (LISA) study evaluated fiuvastatin inpatients with coronary artery disease and hyper-cholesterolaemia and found that itreduced cardiac events by 71%.
What is the role of HMG Co A reductase inhibitors in patients withhypercholesterolaemia and no signs of coronary heart disease?
A recent study from Scotland showed that treatment with pravastatin significantly reduced the incidence of myocardial infarction (30% reduction) and death fromcardiovascular causes (33% reduction) without adversely affecting the risk of death fromnon-cardiovascular causes in men with moderate hypercholesterolaemia and without ahistory of myocardial infarction (N Engl J Med 1995; 333: 1301-7).
What is the role of HMG CeA reductase inhibitors in patients with coronary arterydisease and 'average' cholesterol levels?
The CARE study (Cholesterol and Recurrent Events Trials Investigators) found thatpravastatin lowered rates of coronary events (including fatal events and non-fatalmyocardial infarction) in the majority of the patients with coronary disease who haveaverage cholesterol levels (N Engl J Med 1996; 335: 1001-9).
What is the effect of statins on elevated triglyceride concentrations?
Serum triglycerideconcentrations are reduced by all statins, with atovastatin and simvastatin having thegreatest effect. The higher the baseline concentration of triglycerides, the greater is thereduction induced by statin therapy.
Mention some adverse effects of statins.
· Common: gastrointestinal upset, myalgias and hepatitis.
· Rare: rash, myopathy, peripheral neuropathy, insomnia, bad dreams, difficulty insleeping or concentrating.
What is the effect of meals on statin absorption?
Lovastatin is better absorbed when taken with food whereas pravastatin is best taken onan empty stomach or at bed time. Food has less of an effect on the absorption of otherstatins.
Why are all statins best given in the evening?
Because the rate of endogenous cholesterol synthesis is higher at night. A patient with hypercholesterolaemia on treatment with statins requires further lowering of LDL cholesterol. If the patient's serum HDL is Iow,
what is the preferred second drug you would choose to add to the patient's antilipid regimen?
Nicotinic acid is the preferred second drug. Nicotinic acid usually increases serum HDL concentrations by 30%, fibrates by 10-15%, statins by 5-10% and bile acid resins by1-2% (N Engl J Med 1999; 341:498-511).James Scott, FRS contemporary Professor and Chairman of the Department of Medicine at Hammersmith Hospital, London, is a physician, biochemist and molecularbiologist. He has made a considerable contribution to lipid and cardiovascular research.
